Diagnosis and Testing
A food allergy diagnosis should come from a qualified medical professional. Medical history is the first step in diagnosing a food allergy.
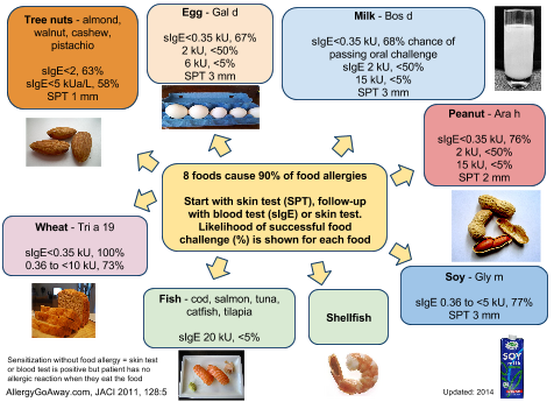
An allergist may then order one or both of the following tests:
Skin prick test – A drop of solution containing the food allergen is placed on your forearm or back, then the skin is gently scratched allowing the solution to go just below the surface of the skin. Results are usually determined within 30 minutes.
*Your allergist will inform you that antihistamines can interfere with skin tests. If stopping your medication for a short time will make your symptoms worse or if you have an extensive rash that prevents skin testing, your doctor may choose to perform a blood test.
Blood test (also known as RAST or ImmunoCap test)– Measures the presence of IgE antibodies to specific foods. IgE is the antibody that triggers food allergy symptoms. Blood samples are sent to a laboratory and may take from several days to a week to determine results.
*Unlike the skin prick test, blood tests are not affected by antihistamines.
Allergists will typically diagnose food allergy based on two out of three positive indicators (case history, skin test, blood test).
Please understand that these tests can't predict the severity of a food allergy.
There is currently no test to indicate how severe your allergic reaction could be so it is advised that you carry epinephrine at all times and practice strict avoidance of the allergen.
An allergist may then order one or both of the following tests:
Skin prick test – A drop of solution containing the food allergen is placed on your forearm or back, then the skin is gently scratched allowing the solution to go just below the surface of the skin. Results are usually determined within 30 minutes.
*Your allergist will inform you that antihistamines can interfere with skin tests. If stopping your medication for a short time will make your symptoms worse or if you have an extensive rash that prevents skin testing, your doctor may choose to perform a blood test.
Blood test (also known as RAST or ImmunoCap test)– Measures the presence of IgE antibodies to specific foods. IgE is the antibody that triggers food allergy symptoms. Blood samples are sent to a laboratory and may take from several days to a week to determine results.
*Unlike the skin prick test, blood tests are not affected by antihistamines.
Allergists will typically diagnose food allergy based on two out of three positive indicators (case history, skin test, blood test).
Please understand that these tests can't predict the severity of a food allergy.
There is currently no test to indicate how severe your allergic reaction could be so it is advised that you carry epinephrine at all times and practice strict avoidance of the allergen.
Oral Food Challenge (OFC)
An oral food challenge is a highly accurate diagnostic test for food allergy and is considered the "Gold Standard" for diagnosis.
Your allergist may recommend that you undergo this challenge for the following reasons:
*to determine a definitive diagnosis based on skin and blood testing
*to confirm results of an inconclusive elimination diet
*to determine if patient has officially outgrown the food allergy (final step)
*to help researchers learn how well participants are responding to treatments in clinical trials
There are three (3) kinds of oral food challenges:
Double-Blind, Placebo-Controlled Food Challenge (DBPCFC)
The patient receives increasing doses of the suspected food allergen OR a placebo (a harmless substance). The allergen and the placebo look alike and neither the patient nor the doctor will know which one is ingested until results are determined – hence the term “double-blind.”
This process ensures that the test results are objective since neither the patient’s anxiety nor the allergist’s preconceptions can influence the outcome.
Single-Blind Food Challenge
The patient receives increasing doses of the suspected food allergen OR a placebo (a harmless substance). The allergen and the placebo look alike and ONLY the doctor knows which one is ingested – hence the term “single-blind.” This process attempts to prevent the patient’s anxiety from influencing the outcome of the test.
Open-Food Challenge
The patient receives increasing doses of the suspected food allergen. Both the patient and the doctor know what allergen is being ingested and is most often done when a patient’s nervousness is unlikely to affect the results.
Your allergist may recommend that you undergo this challenge for the following reasons:
*to determine a definitive diagnosis based on skin and blood testing
*to confirm results of an inconclusive elimination diet
*to determine if patient has officially outgrown the food allergy (final step)
*to help researchers learn how well participants are responding to treatments in clinical trials
There are three (3) kinds of oral food challenges:
Double-Blind, Placebo-Controlled Food Challenge (DBPCFC)
The patient receives increasing doses of the suspected food allergen OR a placebo (a harmless substance). The allergen and the placebo look alike and neither the patient nor the doctor will know which one is ingested until results are determined – hence the term “double-blind.”
This process ensures that the test results are objective since neither the patient’s anxiety nor the allergist’s preconceptions can influence the outcome.
Single-Blind Food Challenge
The patient receives increasing doses of the suspected food allergen OR a placebo (a harmless substance). The allergen and the placebo look alike and ONLY the doctor knows which one is ingested – hence the term “single-blind.” This process attempts to prevent the patient’s anxiety from influencing the outcome of the test.
Open-Food Challenge
The patient receives increasing doses of the suspected food allergen. Both the patient and the doctor know what allergen is being ingested and is most often done when a patient’s nervousness is unlikely to affect the results.
SOURCE:
FARE website at http://www.foodallergy.org
Asthma and Allergy Foundation at http://www.aafa.org
American College of Allergy, Asthma and Immunology at http://www.acaai.org
Image from http://www.allergygoaway.com
Website information should not substitute for seeking responsible, professional medical care.
First created 2012, last updated 2014